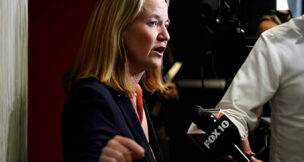Respite centers for homeless are a critical component of the health care system
Guest Opinion//February 10, 2020//
Respite centers for homeless are a critical component of the health care system
Guest Opinion//February 10, 2020//
Maria Pina of Maricopa Association of Governments , left, and Tara Devlin of Community Bridges Inc. , far right, give hand warmers to Tony Cortes, who...